Syndrome X
Patients with a chronic stable pattern of
mixed angina, "ischemic" ST-segment depression, and/or
myocardial perfusion defects during stress test, but angiographically
normal coronary arteries are classified as having syndrome X.
In these patients, angina also predominantly occurs on exertion,
typically with a variable ischemic threshold and occasionally
at rest, but very seldom at night. Although the location and
radiation of pain are often indistinguishable from those of
patients with flow-limiting stenosis, some distinct features
raise the suspicion of syndrome X:
(1) patients usually report persistence of
angina for several minutes after the interruption of exertion,
and many report attacks lasting over 30 mm;
(2) they have a poor response to sublingual
nitrates, which were also shown to worsen exercise tolerance,
in sharp contrast with their established beneficial effect in
patients with flow-limiting stenosis (Fig.
209-1);
(3) they show a variable individual response
to prophylactic long-acting nitrates, calcium antagonists, and
beta blockers, possibly because of differences in the underlying
causes of microvascular dysfunction;
(4) they develop their typical pain (often
with transient ischemic ECG changes) during dipyridamole test
but without development of left ventricular contractile abnormalities
;
(5) they often have an enhanced response to
painful stimuli, which contributes to explain the paradox of
severe angina in the absence of detectable myocardial contractile
dysfunction (Fig.
209-2); and
(6) Holter monitoring demonstrates that some
episodes of chest pam and ST-segment depression are not associated
with tachycardia, and it may show episodes of transient ST-segment
depression in patients with a negative exercise test, suggestive
of possible episodic occurrence of microvascular constriction.
The diagnosis of syndrome X is confirmed by
(1) the evidence of a cardiac origin of pain because of its
consistent association with transient ischemic ECG changes and/or
myocardial perfusion defects during exercise test or by diagnostic
ECG changes on Holter monitoring (cardsynX-fig1.gif);
(2) normal coronary angiogram and
(3) the exclusion of epicardial coronary spasm on the basis
of distinct clinical history, absence of transient episodes
of ST-segment elevation, and failure to induce coronary spasm
by provocative tests.
Maseri,A. and Others, Coronary Blood Flo w
and Myocardial Ischemia ,THE HEART,Hurst's,Volume 1 10th edition
,pp.1124-1125.

CardsynX-fig1.gif
(http://www.hosppract.com/issues/2000/02/kaski.htm)
The Microvasculature and Coronary Ischemia
The recognition of the likely importance of
the coronary microvascular resistance vessels in the pathogenesis
of angina pectoris resulted from studies of patients with angina-like
chest pain and angiographically normal epicardial coronary arteries.
The coronary etiology of the chest pain is
supported by the frequent but not universal evidence of ischemia
in these patients during exercise testing; many were found to
have abnormal vasodilator reserve. Specifically, in patients
with angina and angiographically normal coronary arteries, endothelial-dependent
vasodilatation of the resistance arteries, as reflected in the
responses of CBF (coronary blood flow) to infusion of the endothelial-dependent
vasodilator acetylcholine, was diminished relative to controls
(cardsynX.fig2-gif and cardsynX.fig3-gif).
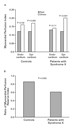
mricardsyn.Fig4gif. Measurements of Myocardial
Perfusion Index in Controls and in Patients with Syndrome X.
Panel A shows the myocardial perfusion index
at rest and during stress. Panel B shows the ratio of subendocardial
to subepicardial myocardial-perfusion reserve index.
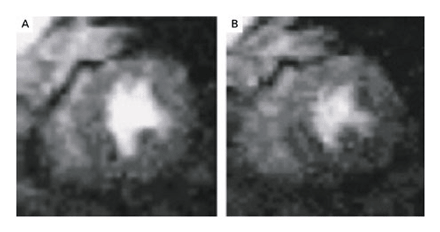
mricardsynX.Fig5-gif. Images of Myocardium
at Peak Myocardial Enhancement during the First Pass of Gadolinium
in a Control Subject at Rest (Panel A) and during Stress (Panel
B), Showing Uniform Myocardial Signal Enhancement.
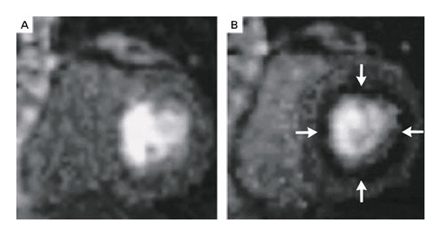
mricardsynX.Fig6-gif. Images of Myocardium
at Peak Myocardial Enhancement during the First Pass of Gadolinium
in a Patient with Syndrome X at Rest (Panel A) and during Stress
(Panel B), Showing a Ring of Delayed Subendocardial Enhancement
(Arrows in Panel B).
In patients with syndrome
X, cardiovascular magnetic resonance imaging demonstrates subendocardial
hypoperfusion during the intravenous administration of adenosine,
which is associated with intense chest pain. These data support
the notion that the chest pain may have an ischemic cause.
In the controls, the
myocardial perfusion index increased in both myocardial layers
with adenosine (in the subendocardium, from a mean [±SD]
of 0.12±0.03 to 0.16±0.03 [P=0.02]; in the subepicardium,
from 0.11±0.02 to 0.17±0.05 [P=0.002]); in patients
with syndrome X, the myocardial perfusion index did not change
significantly in the subendocardium (0.13±0.02 vs. 0.14±0.03,
P=0.11; P=0.09 as compared with controls) but increased in the
subepicardium (from 0.11±0.02 to 0.20±0.04, P<0.001;
P=0.11 for the comparison with controls). Adenosine provoked
chest pain in 95 percent of patients with syndrome X and 40
percent of controls (P<0.001). See mricardsynX.fig4-gif,
mricardsynX.Fig5-gif, and mricardsynX.Fig6-gif.
Although values for
the transmural myocardial perfusion index at base line and under
stress were equivalent between the groups, in the patients with
syndrome X the subendocardial myocardial perfusion index did
not increase with adenosine; in the controls, in contrast, a
normal increase was seen. There was also a significant reduction
in the subendocardial myocardial perfusion index normalized
to heart rate in the patients with syndrome X, which was not
seen in the control group. The responses in the subepicardium
were similar in both groups. Thus, the ratio of subendocardial
to subepicardial myocardial-perfusion reserve index was significantly
lower in patients with syndrome X. There was consistent evidence
in patients with syndrome X of an abnormality of myocardial
perfusion limited to the subendocardium. These results could
be obtained because transmural resolution is higher with cardiovascular
magnetic resonance imaging than with other techniques.
The above results show that patients with
syndrome X have a reduction in subendocardial myocardial perfusion
index normalized to heart rate during stress and a reduction
in the ratio of subendocardial to subepicardial myocardial-perfusion
reserve index. These findings, combined with the occurrence
of chest pain during stress in patients with syndrome X, support
the hypothesis that subendocardial ischemia is the cause of
the angina symptoms in these patients. However, whether there
is an actual absolute reduction in subendocardial perfusion
with stress in patients with syndrome X is unresolved.
http://content.nejm.org/cgi/content/full/346/25/1948
Abnormal Subendocardial Perfusion in Cardiac
Syndrome X Detected by Cardiovascular Magnetic Resonance Imaging
Jonathan R. Panting, M.B., M.R.C.P., Peter D. Gatehouse, Ph.D.,
Guang-Zhong Yang, Ph.D., Frank Grothues, M.D., David N. Firmin,
Ph.D., Peter Collins, M.D., and Dudley J. Pennell, M.D.
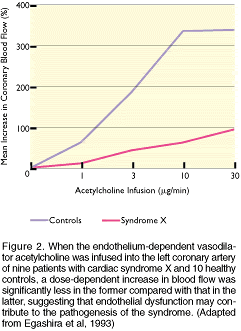
CardsynX-fig2-3.gif
In contrast, the flow responses to the non-endothelial-dependent
dilators, isosorbide dinitrate and papaverine were no different
between patients and controls, suggesting that the intrinsic
vasodilator capacity of the resistance arteries was not defective.
Similar defects in endothelial-dependent increases in CBF have
been observed in LV hypertrophy associated with hypertension,
another condition that may be associated with angina pectoris
with angiographically normal epicardial coronary arteries.
The histopathology of biopsy specimens from
patients with normal epicardial coronaries but with anginal
syndromes has demonstrated capillary narrowing with swollen
endothelium encroaching on the lumen as well as decreased capillary
density. Thus the coronary microvasculature can develop dysfunction
of vasomotor control mechanisms and of endothelial-dependent
vasodilation that may become clinically significant in the setting
of increased demand or MV02. In this situation, the loss of
vasodilator reserve and/or the actual constriction of resistance
arterioles may induce ischemia and chest pain.
O'Rourke,R. and others,Diagnosis and Management
of Patients with Chronic Ischemic Heart Disease,Hurst's THE
HEART,Vol.1,Page1217,10th Edition.
In view of the syndrome's good prognosis, therapeutic goals
should be to control the patient's chest pain and improve quality
of life.
Treatment
As the mechanisms underlying chest pain in
syndrome X probably vary in different subgroups, there is no
standard, off-the-shelf therapeutic protocol. Instead, various
types of drugs and therapeutic approaches have been tested.
Antianginals
Standard antianginal agents are often used
on an empiric basis rather than clear scientific evidence.
Calcium antagonists appear to be beneficial
in a proportion of patients. Nifedipine has been shown to improve
angina and ST-changes as well as to have positive effects on
coronary vasomotor tone, but mainly in patients without increased
sympathetic drive.
Diltiazem is also widely used and is an effective
antianginal agent in syndrome X.
Nitrates, which are extremely effective in
patients with coronary artery disease (CAD), appear to be beneficial
in approximately 40% to 50% of syndrome X patients.
Beta-blockers have been shown to reduce the
number of episodes of chest pain and improve exercise tolerance
mainly in syndrome X patients who have increased sympathetic
activity.
Angiotensin converting-enzyme (ACE) inhibitors
have been tested against the syndrome based on the notion that
the renin-angiotensin system plays an important role in the
regulation of coronary vasomotion and may thus be a pathogenetic
factor. It has been showed that ACE inhibition improved exercise-induced
angina and ECG changes in a small group of patients with microvascular
angina.
Other Agents
Among other treatments to control chest pain
that appear to be effective in some cases, imipramine, a tricyclic
anti-depressant used for management of chronic pain disorders,
has been shown to significantly reduce the number of chest pain
episodes in patients with angina and normal coronary arteries.
However, imipramine is associated with a high incidence of side
effects that may impair the patient's quality of life.
A similar situation may arise with aminophylline,
a competitive blocker of adenosine purinergic receptors that
has been shown to reduce the magnitude of chest pain and ST-segment
changes in syndrome X patients.
Finally, transdermal administration
of 17-beta-estradiol in women with syndrome X reduces the number
of episodes of chest pain during daily activities.But its use
has to be balanced against side effects long term.